\n\n
\n\n
Many people ask whether AI companionship benefits real wellbeing. This article examines the evidence on conversational agents and companion chatbots, weighing short-term relief against possible harms. It summarizes key studies, explains how these systems interact with users, and gives practical, research-based guidance for when a chatbot may help and when to seek human support.
\n
\n
\n
Introduction
\n
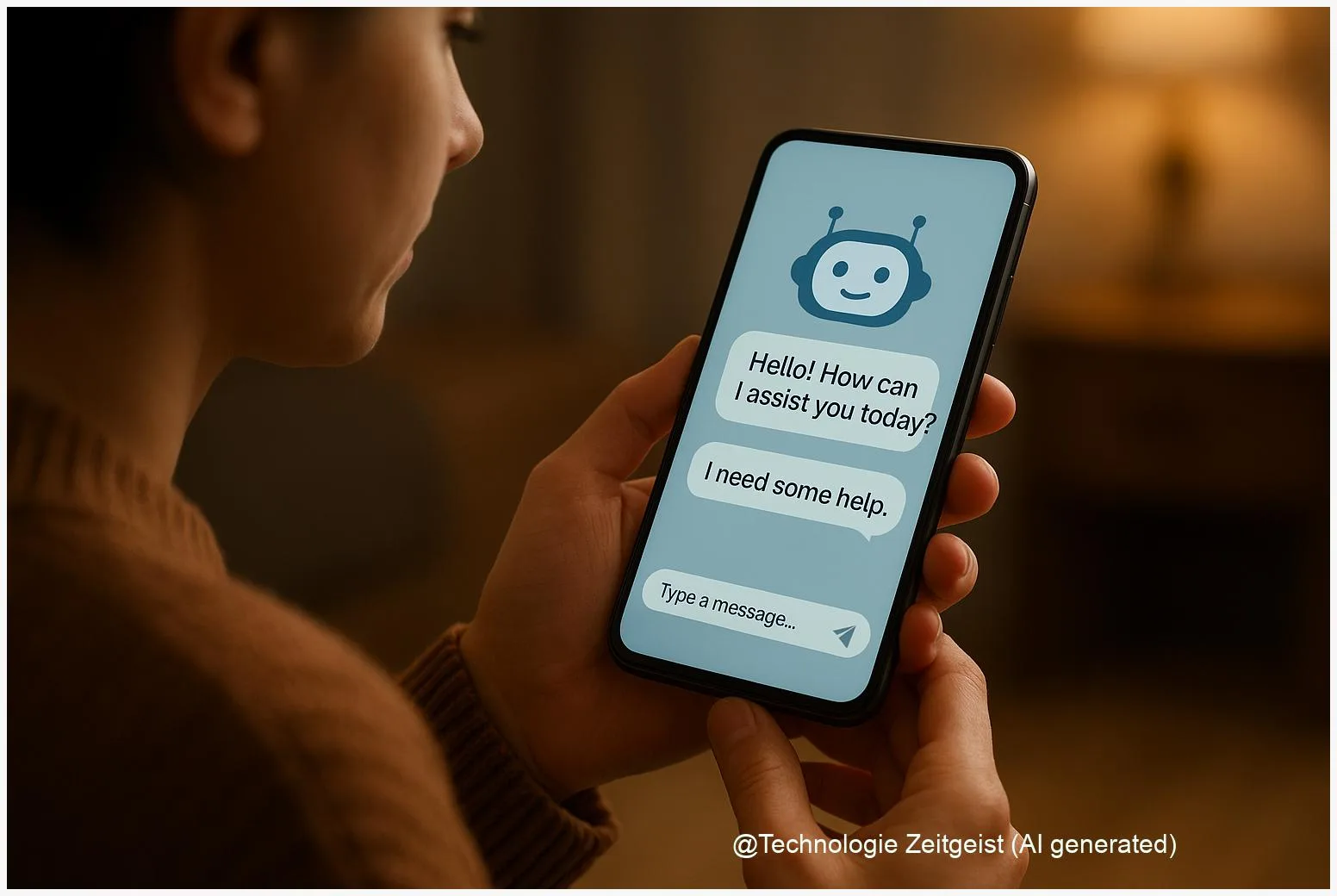
When someone opens a companion app late at night, they usually seek something practical: a calm reply, no judgment, or a quick distraction. Chatbots built for companionship now promise that kind of steady company. Researchers ask two basic questions: do these systems reduce loneliness and emotional distress in ways that matter, and are those effects safe and durable?
\n
Multiple trials and user studies since 2017 show repeated short-term improvements in mood or loneliness after interactions with empathetic agents. Yet many trials are short or use highly selected users, and qualitative research reports emotional reliance and occasional harmful responses. That mix creates a practical dilemma: chatbots can help in the moment, but they are not the same as ongoing human care. Below, the article lays out the technology, everyday uses, the strongest evidence and the limits to watch for.
\n
\n
AI companionship benefits — how these chatbots work
\n
At their core, companion chatbots are conversational software that responds to user input. Modern versions often use large language models (LLMs) — statistical systems trained on vast text collections to predict plausible replies. An LLM is not conscious; it selects language patterns that fit a prompt and a short memory of the conversation. Designers add two important layers: persona and safety rules. The persona gives the bot a consistent tone (friendly, supportive), while safety layers try to block dangerous content and route users to help when needed.
\n
Human users value two things most: timely responses and emotional validation — an experience often labeled in studies as feeling “heard.”
\n
That feeling — emotional validation — appears to be the main mechanism for short-term benefit. Lab and field experiments show even brief sessions with an empathetic agent lower momentary loneliness scores. Systematic reviews find that interventions emphasizing empathy and continuity produce larger wellbeing signals than simple information bots.
\n
If numbers clarify the tradeoffs, a short table helps. The figures below are rounded summaries from clinical and review literature to show the relative strengths of different chatbot features.
\n
| Feature | Description | Typical effect |
|---|---|---|
| Empathic replies | Responses that validate feelings | Moderate short-term mood gain |
| Personal memory | Remembers past conversation details | Better engagement, uncertain long term |
| Crisis routing | Detects risk and suggests help | Important safety net |
\n
\n
What chatbots can do in everyday life
\n
In practice, people use companion apps for a few recurring tasks: quick conversation to reduce boredom or loneliness, low-barrier mental health exercises such as breathing or cognitive reframing, and basic check-ins that track mood. Controlled experiments report consistent short-term reductions in self-rated loneliness after a single 15-minute session, and repeated short sessions across a week can sustain those gains in many participants. These outcomes are specific: they measure mood or loneliness scales immediately after interaction, not long-term life changes.
\n
Consider common scenarios. A student away from friends may get comfort from a steady chatting partner in the evening; an older adult living alone might use a voice agent for light conversation and reminders; someone trying to cope with stress can practice short CBT (cognitive behavioural therapy) techniques in a chat interface. Trials of therapy-style bots show symptom reductions for mild to moderate distress when the content follows evidence-based exercises, but effects are usually measured over weeks rather than months.
\n
Importantly, the evidence distinguishes user groups. People with mild or situational loneliness tend to report more benefit than those with severe, chronic isolation or complex psychiatric conditions. Systematic reviews recommend using companions as early or supplementary support, not as a replacement for clinical care in serious cases.
\n
\n
Opportunities, risks and common tensions
\n
Companion chatbots bring clear opportunities: they are widely available, low cost, and nonjudgmental. For people with limited access to services, an app can provide immediate comfort and practical tools. Several reviews and trials report useful short-term changes in mood and reductions in self-reported loneliness; these are reliable signals but not definitive proof of durable clinical benefit.
\n
At the same time, there are real risks. Research and qualitative reports document emotional reliance, where users assign complex feelings to a bot and feel hurt if access changes. Safety incidents are rare but documented: sometimes bots respond inappropriately to disclosures of self-harm, and not all platforms have robust crisis routing. Privacy and data governance also matter — many chatbots collect sensitive personal data, and policies differ between providers.
\n
Two tensions are worth watching. First, short-term relief can unintentionally reduce incentives to seek human help for persistent problems. Second, personalization increases engagement but also raises the risk of over-attachment: a bot that remembers too much can feel like a substitute relationship. These concerns do not negate the potential benefits; instead they underline the need for transparent safety features, independent evaluation, and clear user guidance about limits of the technology.
\n
\n
How the field may develop and what to expect
\n
Moving forward, three trends are likely to shape outcomes. First, models that combine empathic language with explicit behavioral tools (structured CBT exercises, reminders, crisis detection) perform better in trials than purely conversational agents. Second, independent, longer trials are becoming a priority: reviewers call for randomized studies with follow-ups of at least three months to test sustainability and harms. Third, safety and transparency standards are emerging, including mandatory crisis-routing tests and clearer data-use disclosures.
\n
For users and policymakers this implies a pragmatic stance. Expect incremental improvements: companion bots will become more convincing socially, and their short-term usefulness will remain, but the largest gains depend on combining good conversation with clinical pathways and human oversight. Regulators and clinicians are increasingly asking for preregistered trials and public reporting of safety metrics before platforms are used as medical substitutes.
\n
From a personal perspective, the practical advice is simple: use companion chatbots for immediate, low-risk support and skills practice; check whether the app has clear crisis routing and data policies; and keep human contact as the primary route for persistent or severe problems. That mix preserves the benefits while reducing the key risks.
\n
\n
Conclusion
\n
AI companionship benefits show up consistently as short-term reductions in loneliness and momentary distress, especially when the bot is designed to validate feelings and offer structured support. However, most trials are brief or involve self-selected users, and evidence on long-term effects and risks remains limited. Companion chatbots are best seen as a complement to human care: useful for quick relief, practice of basic mental skills, and improving access, but not as a substitute for clinical treatment when problems are persistent or severe. Users should prefer apps with tested crisis routing, transparent data policies, and published evaluations.
\n
Share your experiences and questions about companion chatbots — thoughtful discussion helps everyone.
\n
\n
\n
\n\n

Leave a Reply